My Postpartum Recovery: How Low Pressure Fitness hypopressives brought ease to my first six months.
In order to give this blog context, I highly recommend that you read my birth story blog where I describe my labor and delivery experience and the state of my pelvis afterwards.
If you don’t want all of the details here is the synopsis: I sustained a grade three tear during delivery and had a grade three bladder prolapse along with a grade 3 rectocele following delivery.
I do wish I had taken slightly better notes about how I progressed myself. However, as best I can recall, this was the progression of my symptoms and the intentional steps that I took to help improve them!
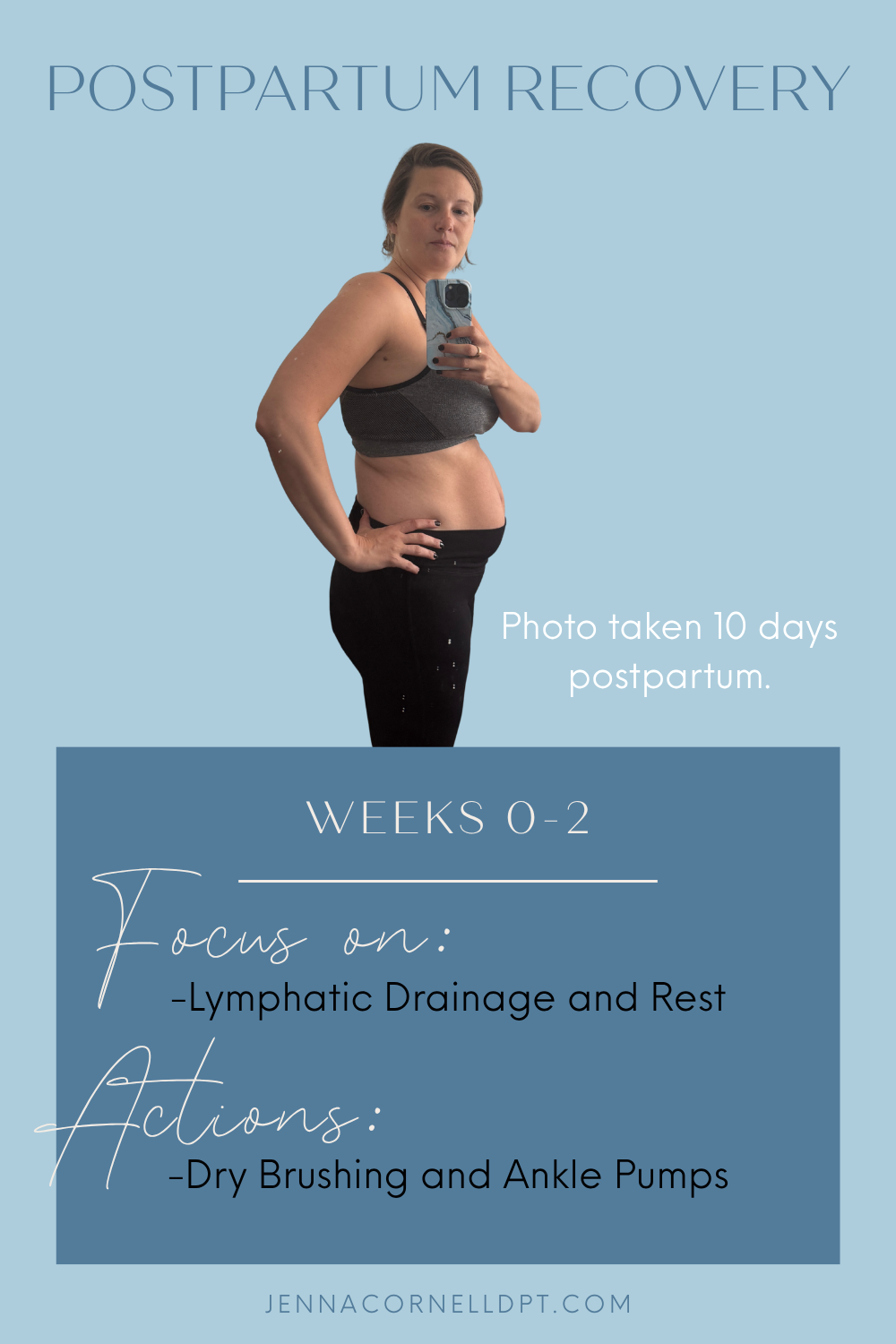
Postpartum Recovery: Weeks 0-2
The first few weeks was the time frame in which my grade 3 tear had the biggest impact. I remember thinking soooo many times “if only this didn’t involve my butt.” Scooting was a challenge and getting up off the couch was really difficult for this reason. I remember being so grateful that my hips were strong and I understood how to optimize squat mechanics and pressure management, otherwise I would have been in trouble.
I remember it being pretty difficult to walk more than short distances for the first two weeks secondary to both the healing tear and the prolapse related heaviness.
7 days postpartum. Annika’s first walk to the park.
I drove while everyone else walked.
I also remember that going to the bathroom would be an ordeal. I had learned following my abdominal surgery that becoming constipated would not help my pelvic situation. I was determined to pass my bowels as normally as possible postpartum and had my first postpartum bowel movement in the hospital. I was grateful that I understood how to best support my perineal body and manage my pressure while having a bowel movement. I can completely understand how this would be hard for most women.
I used a lot of ice diapers throughout this time along with perineal sprays, Motrin and Tylenol. After delivering unmedicated, I initially scoffed at the nurse when she offered me these pain relievers. She scoffed right back at me (lol). I initially declined as I had some concerns about their impact on my gut. However, after about 12 hours I gave in and took them. My pregnancy GI symptoms subsided almost immediately after delivery and the pain from my tear did impact my ability to move somewhat and position myself for feedings. So ultimately I embraced it.
My focus during this time was rest and optimizing lymphatic drainage. I had swelling in my legs immediately postpartum. I had very minimal swelling during pregnancy, but in the first week postpartum my left leg was obviously swollen. Your pelvic floor plays a big role in lymphatic drainage and I suspect the swelling may have been present on that side because my tearing was more extensive on the left. I am sure that my mostly sedentary state throughout this time period did not help. I dry brushed daily and performed ankle pumps throughout the day in order to encourage lymphatic drainage from this area.
I did have help during this time. My husband stayed home for the first week and several days during the second week. My mother and mother-in-law also came to help a bit during the second week. I believe I had one day during the second week where I was on my own. Honestly, I probably had no business being on my own at that point and I do think it likely did impede my recovery a bit. If I had not torn I probably would not have felt as reliant on people during this phase. However, I do believe that for most women as much rest as possible would be generally beneficial throughout this time.
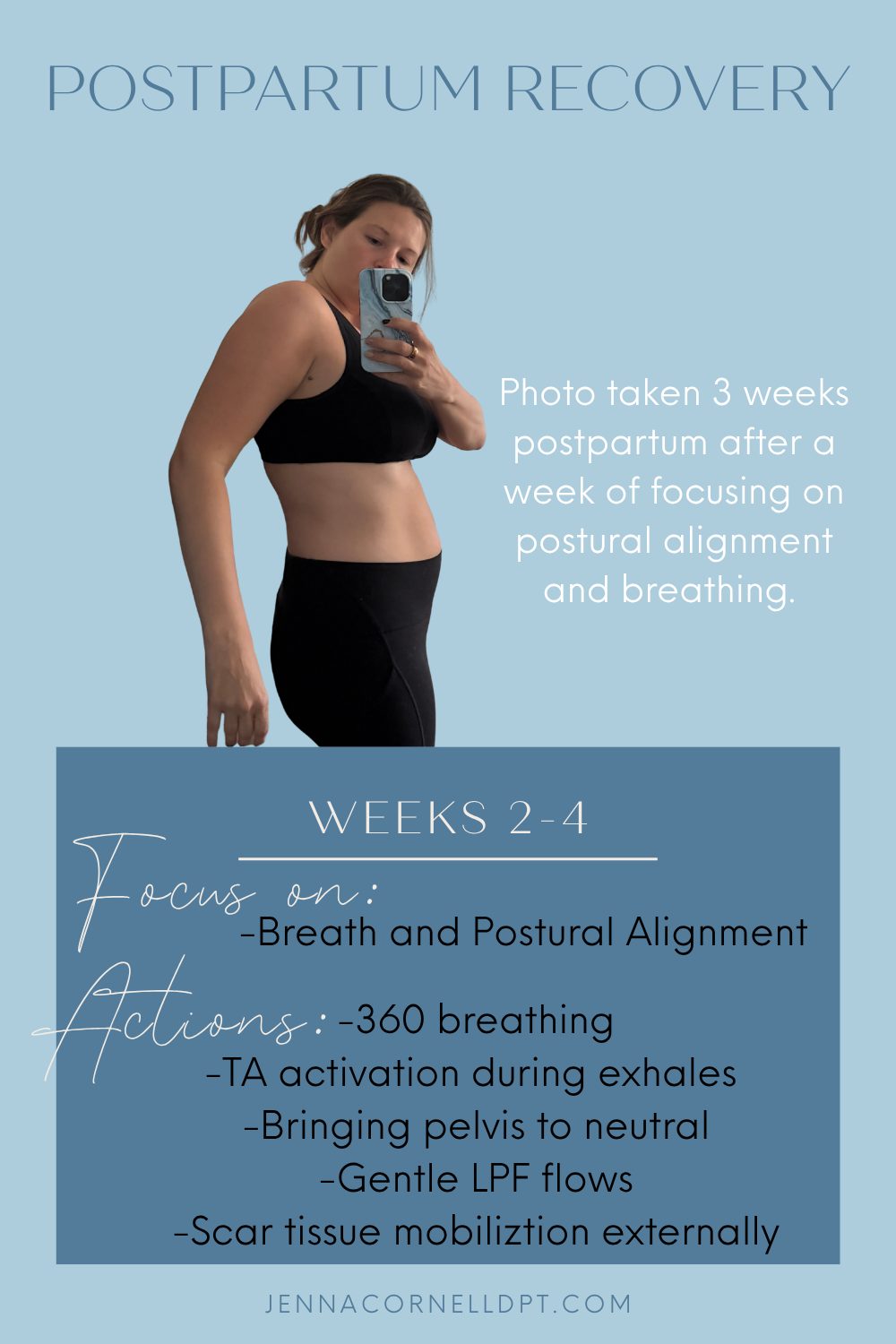
Postpartum Recovery: Weeks 2-4
I began to be able to scoot a little better and stopped needing as much pain control. I continued to abstain from walking more than household distances as it would result in a noticeable increase in my pelvic heaviness and the soreness in my perineum.
I started to bring intention to my breath and posture.
I focused on opening my back during 360 breathing. During my inhales I would think about emptying from the bottom up to encourage some TA (deep ab) activation. Thankfully my TA did not seem to be inhibited postpartum and I had very little diastasis recti.
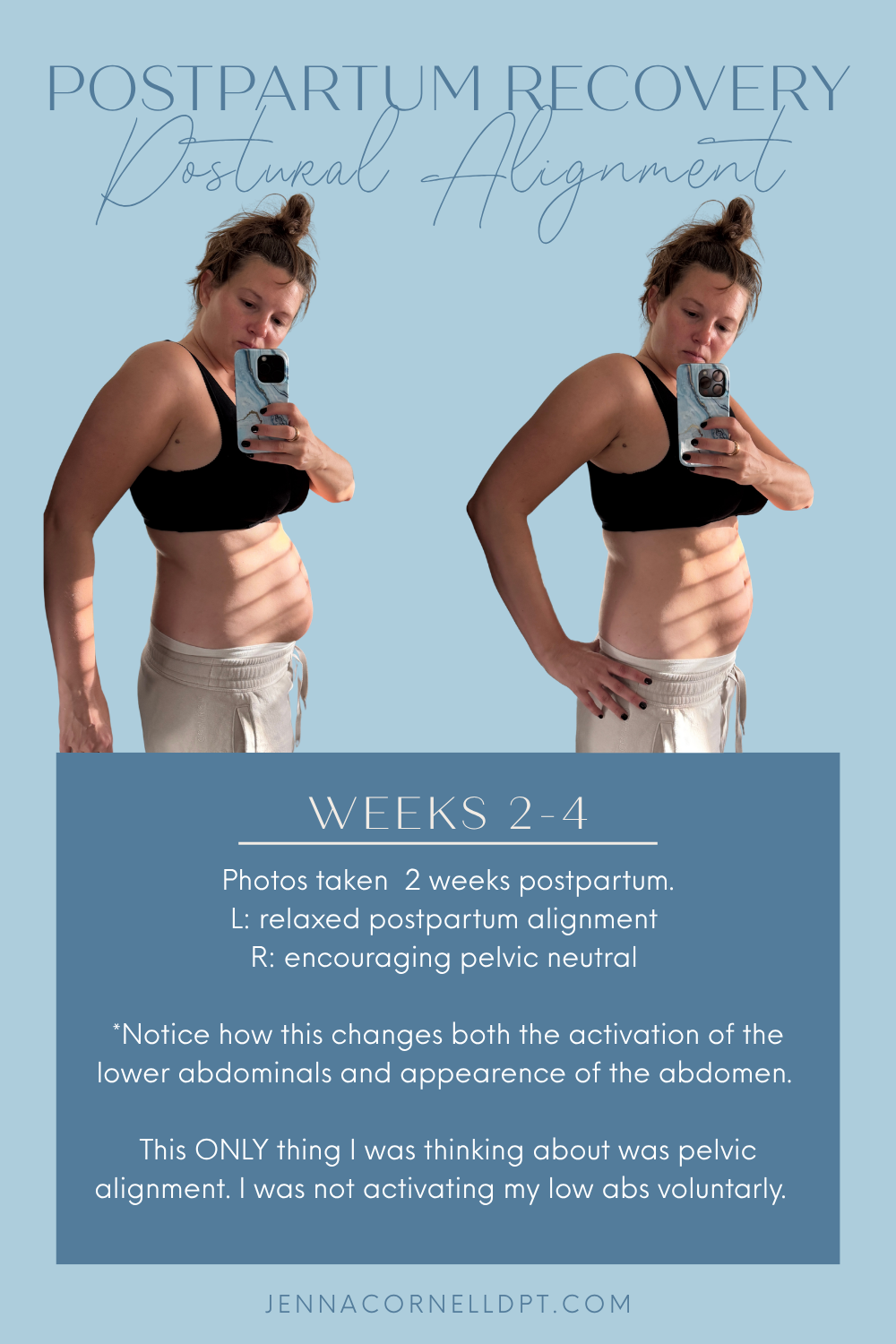
I also increased my postural awareness. My main focus was working my pelvis back toward neutral and finding the length in my back to stack my ribcage over my pelvis.I genuinely feel this is a super important step postpartum that most women probably skip. I never forced anything, but gently started making neutral posture available to my body. I knew that if I could start to improve my posture it would change the way my body handled pressure and would help decrease my prolapse symptoms in the long run. It also encouraged my lower abdomen to work as well.
To combine all of these things I started doing some gentle LPF flows. I have my first flow recorded on October 9th. In general it is not recommended to do the hypopressive maneuver until 6 weeks postpartum in order to allow your uterus to return to its normal size and position before it is “lifted” with the hypopressive. I followed this rule and did not incorporate it during this time period. However, I still felt that breathing in the Low Pressure Fitness postures was super helpful for mobilizing fascia that had become restricted throughout both pregnancy and my immediate postpartum time period.
Picture from my first Low Pressure Fitness flow postpartum. My primary focus was postural alignment.
I also started doing some scar tissue mobilization to my perineum externally. As I mentioned above, my tearing was more significant on the left side and at times I could feel a pull in this area. I began mobilizing any tightness that I could sense around this area and into my inner thigh. Additionally I began to mobilize some of the scar tissue from the stitching in the perineal body. I used Earth MaMa’s perineal balm to aid with this.
My prolapse stayed pretty steady visually throughout this time with them being around a grade 3 in standing at the end of the day.
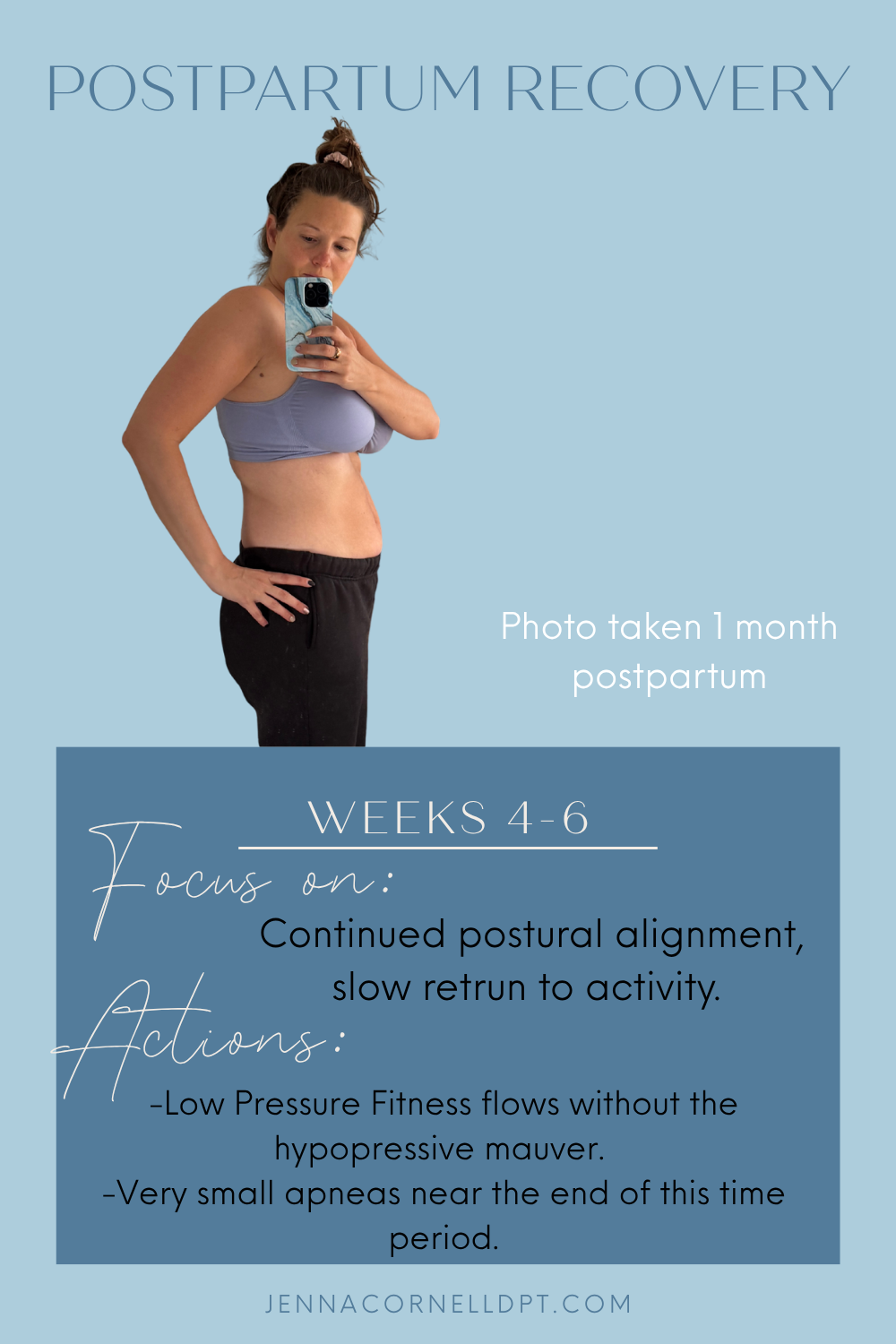
Postpartum Recovery Weeks 4-6
I continued to progress slowly throughout this time.
My prolapse symptoms improved but only slightly. I started to be able to move around the house pretty well and perform light ADL's without a notable increase in the feeling of pressure. However, baby wearing would increase symptoms along with any attempts to walk more than household distances. I continued to have the feeling of heaviness, however I was able to do more before it became noticeable and generally it would only “come on” at the end of the day or if I attempted something mentioned above.
Visually not much changed with my prolapse. I continued to have visible grade 3 decent in standing at the end of the day.
I continued to work gently on my scar tissue, which did slowly improve throughout this time period.
My Low Pressure Fitness flows continued to focus on improving the postural alignment of my pelvis and ribcage and to strengthen my abs with my breath. Near the end of this time period I did start to feel as though I was ready to perform the hypopressive maneuver. I started playing around with opening my ribcage during an apnea but refrained from opening to the extent that the lift would reach my pelvis in a significant way. By the time I hit 6 weeks I was ready to fully return to hypopressive exercise.
Weeks 6-12: The Effect of Hypopressive Exercise on Postpartum Recovery
I was officially six weeks postpartum on November 2nd, which also happens to be my birthday. I was beyond excited to fully return to the hypopressive maneuver.
I had certain expectations for how it would influence my symptoms. It honestly was everything I hoped it would be and more.
My very first postpartum hypopressive manuver at 6 weeks.
I knew I would have some improvement in my cystocele. One of the mechanisms that is thought to improve prolapse is the connection to the urachus ligament. This ligament runs from your belly button to your bladder. As your belly button lifts you can expect a lift in your bladder. The potential mechanism of improving rectocele is less clear, with possible theories including impact through fascial connections, or the facilitation of a relative negative pressure state in the abdomen. I had seen improvement in rectoceles in my practice, but I would admit that sometimes they took a bit longer to come around than cystoceles.
However, the change in my prolapse symptoms was significant and relatively quick. I took my first solo walk for exercise on November 6th, pushing a stroller and handling the dog, just a few days after implementing the hypopressives. My memory is a bit blurry but on December 3rd I drove to the mall to get out of the house and walk. I don’t remember even considering an increase in prolapse symptoms as a potential consequence at that time.
First postpartum walk by myself.
I also continued to self examine my prolapse at the end of the day. At the 6 to 7 week mark it continued to be pretty visible.
However, it was cool to observe the change in the tissue position while performing the hypopressive maneuver. I had observed this a little bit with clients as they were first learning the maneuver. However, generally in my practice I don’t do internal work/exams without a clear benefit/indication to the client. So typically, by the time someone truly masters the hypopressive they have enough of a symptom reduction that they no longer require internal work. I had not seen too many examples of the lift a really well done hypopressive maneuver can create.
It is profound. I was actually impressed. And I had pretty high expectations. When I say Low Pressure Fitness can disappear your prolapse, I’m not exaggerating.
Occasionally I have seen critics dismiss hypopressives because the medical literature has not made the mechanism abundantly clear. In fact, many renowned pelvic PT’s will dismiss it all together. As a PT I hope that someday we will have a full understanding of the mechanism. However, as a postpartum mom, I frankly don’t actually care what the true biological mechanism is, all I know is that it works.
Eventually, somewhere within this time frame I stopped thinking about my prolapse all together. The last time I remember checking, which was somewhere in this timeframe, my rectocele had disappeared completely and my bladder prolapse would be considered a grade one at the end of the day in standing. Subjectively, my symptoms of pressure and post void dribble disappeared. By the time I went to Florida in January I literally didn't give it any thought.
In apnea at 10 weeks.
Annika enjoying the practice with me.
My prolapse symptoms were not the only thing that improved with my initiation of the hypopressive maneuver. I also noticed a significant improvement in my scar tissue mobility. I was not expecting this to the extent that I experienced this. I vividly remember feeling a release in the left side of my perineum while performing one of my early hypopressive maneuvers. I believe this is because the hypopressive maneuver influences the pelvic floor ALONG with its fascial connections. This release was deep enough that it would not have been achieved with any type of external mobilization.
I am forever grateful to Low Pressure Fitness and hypopressive exercise for giving me such profound results with pretty minimal effort.
Postpartum recovery: Months 3-6
Honestly, pelvic symptoms have been the least of my problems over the last three months.
One of the things that I struggled with in early postpartum was numbness in my hands during night feedings. I ended up with continued numbness in my L fingers and a gnarly resurgence of thumb issues on my R hand. Due to the pain in my hands and wrists I did not spend a lot of time in the quadruped position in LPF and don’t think that my upper body strengthening was enough to combat the increasing weight of my baby and continued nursing. I ended up with some significant neck pain in this period that did not improve with my Low Pressure Fitness training.
I finally got pretty serious about improving this situation around 5 months and began incorporating some rehab type exercises for my neck and upper body. I came to terms with the fact that if I could not strengthen my body in a closed chain position I needed to pick up some free weights. I have been utilizing some barre style workouts on YouTube to keep me motivated.
Additionally I began to suspect that I was having a bit of an autoimmune flare postpartum due to generalized joint pain and stiffness. Blood work confirmed that, at the very least, I have a positive ANA again.
I was able to pretty much eat whatever I wanted while I was pregnant(with the exception of gluten, which I did not try) without consequence. I very quickly adjusted to having nightshades, dairy and oats be a part of my diet. Unfortunately, I don’t seem to be able to tolerate these things any longer. So I am adjusting to that and have made some changes with the intention of beginning the Autoimmune Paleo protocol if I do not see improvement.
So far a combination of specific exercise, generalized upper body training and dietary changes seem to be helping the neck situation.
I have continued my Low Pressure Fitness practice about 4x a week throughout this time period for the following reasons:
I love it and I will do it forever
I continue to have some fascial tightness in my back due to postpartum changes, this is continuing to improve but is not yet back to my pre-baby alignment. I am motivated to change this for both functional and aesthetic reasons.
The breath work is wonderful for my nervous system. As a new mother I often have felt like I am managing the nervous system of the whole household. I am grateful to have this as a tool to help me carry that pressure.
I know that my pelvic and abdominal tissues are still recovering and sense that this time period continues to be important for my long term pelvic health. I don’t have symptoms and I hope to keep it that way.
My Postpartum Mindset
Overall at 6 months I am very pleased with how I feel. My pelvis has healed beautifully. My challenges are mostly autoimmune related and the orthopedic concerns seem to be responding in a positive way.
I believe my ease of healing was due to the work I put in prior to becoming pregnant. My pelvic floor and core coordination were on point and I never lost that coordination.
I really appreciate that this part has been easy postpartum. I can’t help but feel a bit sad that women truly struggle in this area. I believe a lot of the struggle could be prevented with some thoughtful connection to the pelvic area while you are trying to conceive.
I also can’t help but wonder what would have happened if I waited until later in my postpartum period to begin influencing my pelvis with the hypopressive maneuver. I have seen improvement for clients in all ages and timeframes. However I suspect there is something special that happens when you influence your tissue in this way from weeks 6-12 due to the general stages of tissue healing.
Stages of Tissue Healing
Typically tissue healing is thought to have 3 phases.
The first phase typically lasts 48ish hours and is known as the acute healing phase. During this phase your body creates inflammation (in a good way!) to bring cells to clear out damaged tissue.
For soft tissue, the second phase typically lasts about 12 weeks. During this phase your body creates its initial scar tissue.
The third phase typically is thought to last 9-18 months and during this phase your body continues to refine the scar tissue that was laid down.
I would argue that scar tissue can be refined indefinitely, but it just takes longer as time passes.
However, I do think there is something to be said about influencing the soft tissue around your pelvic organs with a hypopressive maneuver during the initial scar tissue formation phase. I explained in my prolapse blog (the various mechanisms of support for your pelvic organs, including ligaments, fascia and pelvic floor. ALL of these tissues are healing and reorganizing postpartum. I suspect (but admittedly have no evidence) that if these tissues are not “lifted” during this time, that the initial scar tissue may not be at the optimal length to give support. Performing the hypopressive may help to encourage formation of scar tissue that is more supportive, making it easier to feel better quickly. Once the first 12 weeks pass I suspect it may take longer to create change.
Once again, I feel like this is a strong reason to learn this method prior to becoming pregnant. Squeezing this in postpartum when you know what you are doing is certainly doable, but it can be a lot to learn upfront.
However, it is never ever too late and I have seen remarkable improvement in women in their 70’s. So if you missed the 12 week window don’t let that stop you from giving it a try!
“Bouncing Back” Postpartum: My Thoughts
For the majority of the last 10 years I have cared far more about how I feel and how my body performs than what I look like.
This focus on performance has held true postpartum. I am exclusively breastfeeding and my priority in this season is to maintain my milk supply and feel strong enough to engage with Annika in the way I desire.
With that being said, I also desire to feel confident and vibrant in this season. I do believe that confidence is mostly an internal job, however liking what you see when you look in the mirror is helpful.
I could write a whole blog post on the psychological mess that is bounce back culture but here is the short version: our bodies do amazing things when we create and birth a baby. It feels like they should be allowed to be a bit different afterwards AND I also completely understand the urge to feel “normal” again. I also believe that motherhood is an athletic event and physical strength is important in a postpartum season.
I think that is a huge win if we can facilitate strength and confidence without stress postpartum.
Again, feeling confident without the pressure. The problem is, most of what we have been taught about obtaining an “optimal” aesthetic can be pretty detrimental postpartum. Cutting calories and high pressure exercises are a sure way to sabotage your healing. I truly believe that most women could feel much better in their skin if they gently corrected their posture and core strength with Low Pressure Fitness, all without creating undue stress during this potentially stressful time period.
I shared some photos to document my progress throughout this blog. My goal in doing so was to provide a realistic expectation of progress and to show changes in posture.
Even now as I write this I am now 7 months postpartum (yes it took me a whole month to fully write this blog). I am pretty pleased with how I look. My clothes are fitting better and I had no problem putting on a 2 piece bathing suit on our recent cruise. I know that I still have some postural things to fine tune and as I do so my figure will continue to “improve”. I also know that it will take a bit of time for my skin to fully return to normal. However, I have full faith that it will.
Overall I wish that most women would allow their body to gently find its strength during this time period. It is a true opportunity to connect with, rather than try to control, your body.
If you are looking for a way to recover, regain confidence and strength, and completely cancel any pelvis symptoms that you might have, I would encourage you to give Low Pressure Fitness a try.
Here are some options for getting started:
Hypopressive Exercise Online Classes
I teach several live classes a week. I highly recommend that you start with an “Intro to LPF: Breath” class if you are able!
Hypopressive Exercise Online Courses
If live classes simply are not in the cards for you during this season I have 2 different online courses that contain everything that you need to implement Low Pressure Fitness hypopressive exercise.
Core Shift is my original course that walks you through the practice step by step. IGNITE us a 30 day challenge program. Honestly both courses are great and which one you choose is a matter of preference.
The Hypopressive Project Online Membership
If you would like access to everything including all courses and live classes, I highly recommend The Hypopressive Project All Access Membership. I created this membership to be the ultimate, accessible resource to help you get started and grow your hypopressive exercise practice. I would be honored if you would join me there!
I hope to see you in class soon!
-Jenna