My Birth Story: an Unmedicated Hospital Birth
I sat down to write a blog post about my postpartum recovery at the six month point.
In my attempt to give a brief context this is what came out.
Early postpartum recovery.
I truly believe that context is important when we talk about postpartum recovery. As humans we are always tempted to compare ourselves to others. However, we all have very different starting points and contexts in which we heal. This context is influenced by our pregnancy and birth experiences. It is also influenced by the support we may or may not have as we recover along with any responsibility that we carry, beyond caring for a newborn, throughout the postpartum period.
I wanted there to be context about my “starting point” as I was recounting my “progress.” It turns out that I failed to make the context brief. So here is my full, detailed, more than you would actually ever want to know, birth story.
I do think that writing it out was therapeutic for me, but I also hope that it serves you in some way.
Disclaimer: I am a pelvic health therapist. In general, when it comes to any bodily function there is no “TMI” in my world. With that being said, in this blog I openly share about my labor and delivery experience along with details about the state of my pelvis. If you know me in real life, and you don’t want to know these things about me, I’d skip this one.
What I Did to Prepare for Labor and Delivery
I had a lot of ideas about what I would do to prepare for labor and delivery. I wanted to explore all of the preparation programs that clients had ever asked me about. I would have loved to eat the most nourishing diet full of organ meats, healthy fats, choline, veggies and fruits. I fully intended to support myself with acupuncture and preparatory tinctures.
The reality was a bit different than my best case scenario. I ended up being nauseous for the majority of my pregnancy. I spent the first trimester on the couch hardly able to keep anything down. My goal was some semblance of nourishment and hydration. By the time I started to feel “better” it was close to 20 weeks and I was epically behind on all things preparing for a baby.
So I kept it pretty simple.
I had regular chiropractic care from a Webster trained chiropractor that I was established with prior to pregnancy.
I continued regular body work with a massage therapist.
I restarted my Low Pressure Fitness practice around 16 weeks and continued until I went into labor. If I am being really honest I probably only did this an average of 2-3 times a week. Throughout my third trimester I integrated a good bit of hip opening, deep squatting and asymmetrical work. I also worked breathing in potential labor positions into my flows.
I intended to do the spinning babies routine, but after a few days of that I was bored and felt like the LPF positions targeted the goals of spinning babies anyway.
I did *attempt* to drink red raspberry tea in my 3rd trimester and I did eat quite a few dates.
I also did perineal massage about 4 times a week from 35 weeks on.
I fully embraced my femininity both physically and energetically throughout pregnancy.
Mentally I did a lot of breath work and visualization. I had intuitively enrolled in Alpha Femme’s Femme Fatale program prior to becoming pregnant. I remember telling my husband it would “make me a better mother” when justifying the investment to him. The timing of the program ended up being truly divine. The first call took place the same day as my first prenatal appointment and the final call took place a few days after I got home from the hospital. It included components involving body and pelvic awareness, feminine energetics, lineage healing work and vocalizing. Although it is not meant to be, it truly was such a beautiful preparation for both delivery and motherhood.
Additionally, my doula also recommended reading Ina May's Guide to Childbirth book which I also found helpful mentally.
Overall I genuinely feel I did the best I had the capacity for.
However, if there is a next time, I am going to try to prioritize acupuncture as I believe it likely would have helped with nausea. Additionally I would love to learn as much as I could from Katie Donnelly (https://thepilatesdoula.com/). I had always admired her offerings when we both worked at The Restoration Space and was excited to have my chance to experience them. However, I was just too sick to follow through with that. Hopefully next time!
Choosing My Birth Team
One of the benefits to working in the pelvic health space was my patients were constantly giving me unsolicited OB and midwife reviews. I heard the good, the bad and the ugly about pretty much every local option from traditional OB to home birth.
The option that had consistent positive reviews was delivering with midwives in a hospital. Unfortunately, this was not available immediately local to me, but I had several clients that “made the drive” to work with WomanWise Midwifery who deliver at Einstein Montgomery Hospital. This felt like the best option, despite the fact that the hospital was a 50 minute drive. I loved the idea of having the support of the midwives for both my prenatal and L&D experience along with the hospital facilities in case I would need them. The icing on the cake was that both the midwife group and hospital were in network with my semi-restrictive HMO insurance plan.
I did elect to hire a doula (roslyngracebirth.com) for additional support. My goal was to deliver unmedicated. It was important to me that there was someone present that was willing and able to provide hands on pain management at all times. My husband was willing, but clueless. My midwives were a bit unclear about exactly how much hands on care they would provide. Additionally, it was always possible that I would not be their only patient admitted. They assured me it was very rare that they had more than one patient admitted at a time. However, this was not guaranteed. I had peace of mind knowing the doula would be there to support both Tanner and I.
It turned out to be a wonderful decision for many reasons, including that I was not my midwife's only patient delivering that day.
My Early Labor Experience
My due date was September 16th.
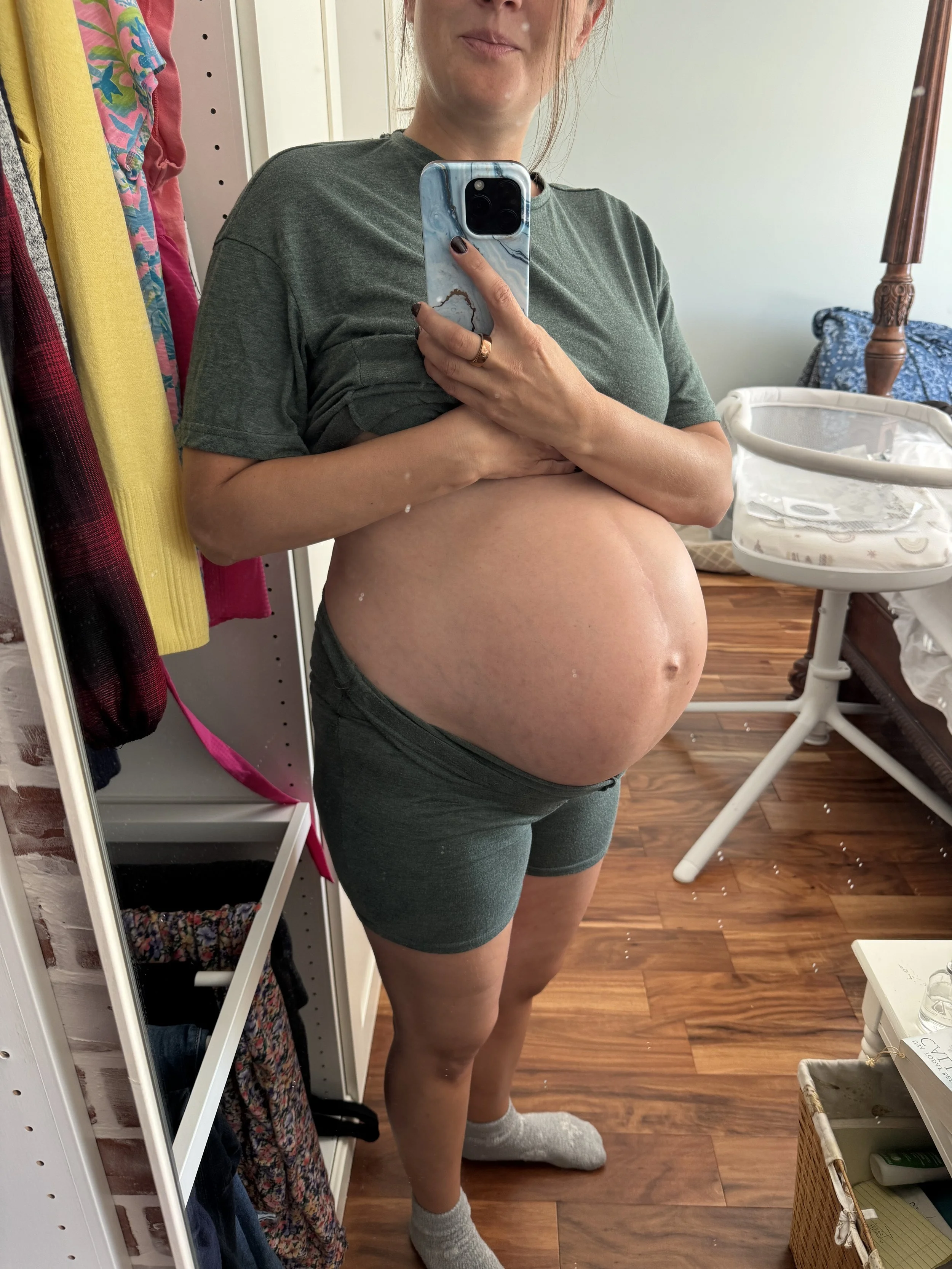
In retrospect I am not sure when you would say I “went into labor.” I experienced rather intense Braxton Hicks and pre-labor contractions in the weeks leading up to my delivery. The only reason I suspected something may have been different on the morning of the 20th was that I had a “bloody show” when I got up to use the bathroom at 5am. This sign of potential progress made me pretty excited being that I was overdue and very hopeful that I would be able to go into labor spontaneously. I tried to rest but I don’t think I was able to go back to sleep.
My belly the day before I went into labor.
I had a lot of difficulty timing my contractions. I was able to walk the dog that morning, but had to stop a few times to let contractions pass. I texted my doula who advised me that what I was experiencing was likely “pre labor”. She encouraged me to try to go about my day as normally as I could.
My mother was scheduled to come over to help me prepare some freezer meals and we decided we would proceed with that plan. I decided to do my nails and hair as I waited for my mom. I wanted to look presentable if I ended up going to the hospital. In retrospect this was a fools errand as my hair and makeup did not come anywhere close to withstanding labor. However, from a mental standpoint it was helpful to imagine I was beautiful throughout the labor process.
As I was doing my hair, I needed to stop and get on my hands and knees on the bathroom floor to manage the contractions. My husband felt that this probably was not normal and encouraged me to tell the doula to “come now.”
In retrospect it obviously was not “normal”. However my contractions were not a typical pattern. I would have a contraction that would last much longer than 1 minute, sometimes up to three minutes, and my time between contractions remained pretty variable. My understanding was that a contraction pattern like this is typically pre-labor. I was told by many sources, including my midwives and dr. google that, when I entered active labor my contractions would take on a consistent pattern. I was told not to go to the hospital until they were at a 4 (or 5) /1/1 pattern. It was emphasized that going to the hospital prematurely may result in my not being admitted or could decrease my odds of unmedicated delivery. Given that it was a 50 minute ride to the hospital I didn’t want to go too early and be turned away. My contractions were much more of a 3-5/1-3/? pattern.
If I had waited for a nice predictable contraction pattern I would have had the baby at home. Predictable contractions never came and I continued to be blessed with looooooonnnnngggggg contractions with minimal (sometimes 15-30 second) breaks between the contractions.
My doula arrived in the late morning, shortly after my mother. Around 12:30pm she suggested that we leave for the hospital due to the intensity and consistency of the contractions. I remember trying to eat in the car but spent most of the time just focusing on my breath. As I mentioned above, we had very intentionally selected a hospital that was about 50 minutes away from home. We arrived at the hospital around 1:30pm.
I remember imagining that I would walk up to the L&D unit through the visitors entrance. However, we opted to go to the ED entrance and I was unable to walk from the car to the door without stopping constantly to let the contractions pass. They (I honestly don’t remember who) saw me and met me in the parking lot with a wheelchair and I gratefully accepted a ride to triage.
I consented to a cervical check in triage and was 6cm upon arrival. I was in triage for an hour. I was vocalizing pretty freely at this point, much to the distress of both the triage nurses and the girl adjacent to me in triage. I still had some ability to take in my surroundings and I remember hearing the triage nurses worry that I wasn’t going to make it to a delivery room. Apparently they were having trouble allocating a L&D nurse for me which is why I was in there so long.
I remember this hour being one of the more painful hours prior to pushing. I think this was because I was unable to truly let go in my mind and I was unable to move freely. I was certainly glad when I was finally given the green flag to move to a labor and delivery room.
My Labor and Delivery Intentions:
I entered labor with equal parts stubbornness and surrender.
I approached birth with firm but flexible intentions. I knew what I desired and was willing to be uncomfortable for it. I was unwilling to let anyone “talk me into” something that I did not want. At the same time, I gave myself permission to change my mind. My mother has often described me as “strong willed”. I was 99% confident that I would be completely fine unmedicated, but I also acknowledged that I wouldn’t know until I was in it. I had established beforehand that if it was significantly “worse” than I imagined I would allow myself to change my mind. The hospital where I delivered had many of my afterbirth intentions as standard of care and I was grateful to have my doula there as an advocate as well.
My mother in law has told me numerous times over the years that my husband was the worst of her four boys to deliver. He has a rather large head and she reflected many times that his head was hard to get out. Our baby's head was measuring in a high percentile compared to the rest of her body at our 34 week ultrasound. However, my friend Becca assured me that those measurements had very little reliability, so I tried not to think too much about it going into delivery.
My birth plan read as follows:
LABOR & DELIVERY
General
I desire a spontaneous, physiological birth
No medication unless aware and provide consent (preference for no epidural, labor stimulates, or narcotics, open to using nitrous oxide)
No IV unless medically indicated
Would like to delay placement of heparin lock if possible (this is the one thing I did end up getting “talked in to” and honestly it didn’t bother me throughout labor like I was concerned it would. However, they did not remove it throughout my entire hospital stay, and that DID bother me. In retrospect I wish I would have advocated harder for its removal.)
No residents/students present
Ambience
Quiet preferred
No bright/florescent lights
Music, diffuser and ambiance lighting present
Minimal interruptions
Comfort
I will wear my own clothes (assuming I bring them), eat, drink and move freely
Pain managed primarily by massage, shower, birthing ball, peanut ball, breathing, position changes, TENS. Open to nitrous oxide.
Husband and doula (Roslyn Cuce) present for support and comfort.
Exams
Always request consent before exams
Will likely want to keep exams to a minimum
Fetal Monitoring
Intermittent fetal monitoring with doppler is preferred
Active Labor
I would like to push in the position of my choosing
No coaching during pushing unless I request it
No artificial breaking of waters
Avoid episiotomy, forceps, and vacuum
AFTER BIRTH
Immediately After Birth
Place baby on chest for immediate skin to skin
Keep vernix on baby, no wiping down
If baby needs help breathing it will be done on me if possible
Keep cord intact until it stops pulsing
No tests, weighing etc performed until after Golden Hour and baby has successfully nursed.
Placenta
Allow the placenta to deliver on its own
No pitocin post birth unless medically indicated
Placenta to be given to doula for imprint
I will not be keeping the placenta
Umbilical Cord
Again, cord remains in place, unclamped, until it stops pulsing
Husband given opportunity to cut the cord
My Early Labor and Transition Experience
There is certainly a part of me that wishes that the triage nurses' fears were warranted. However, my labor was not short.
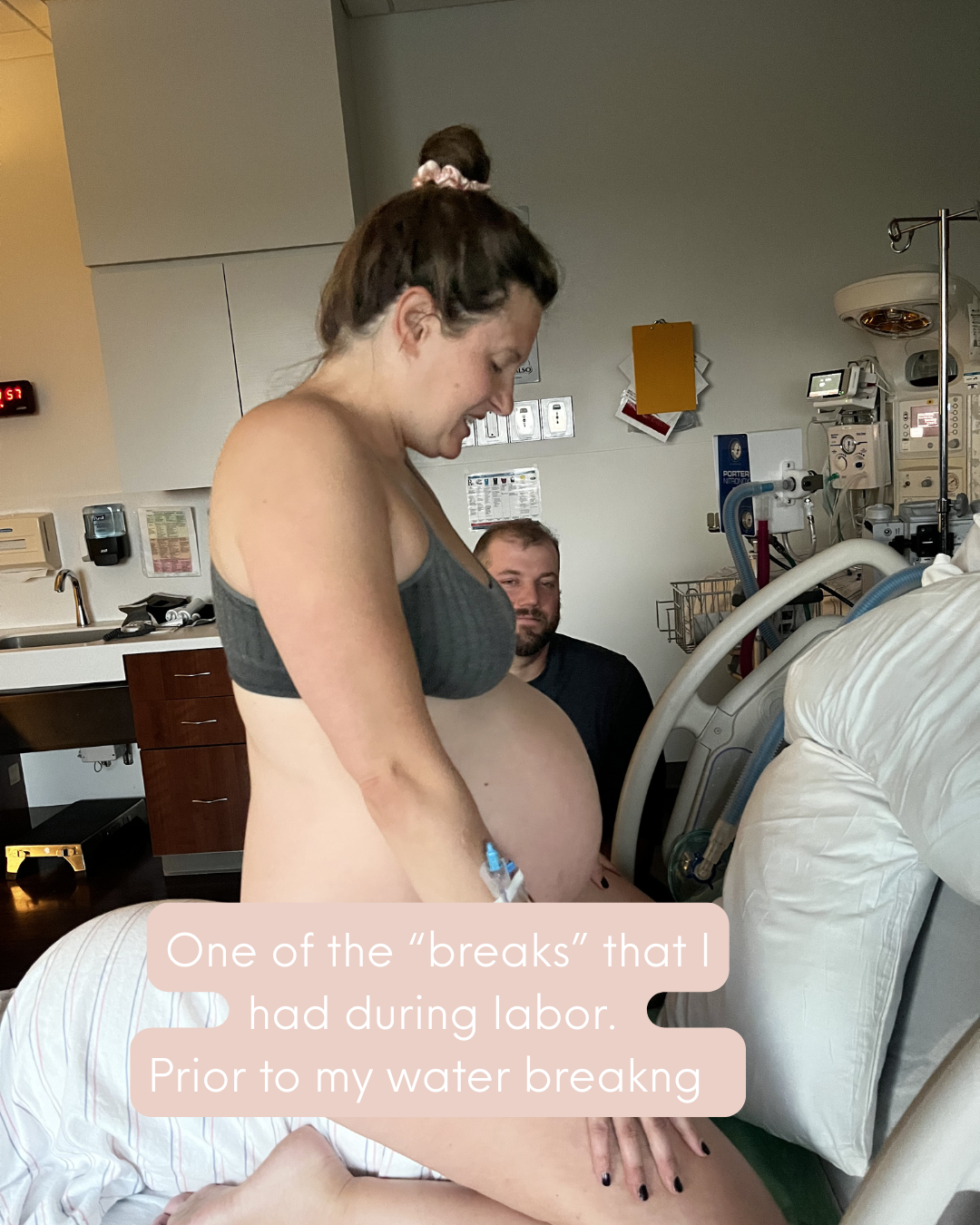
I was moved into a delivery room around 2:30pm. My contractions continued to be long with minimal rest in between. However, after being moved to the delivery room I was able to truly follow my body's desires for movement and positioning. I also entered an altered state of consciousness. I credit my birth team for creating an environment in which I felt safe to depart reality in this way. I trusted that both my husband and my doula understood my desires for the birthing process and would advocate for them should they be threatened in any way.
When I say I entered a different state of consciousness, I truly feel like I was on a different planet for most of labor. I felt as though I was communicating with the baby inside of me along with deeper parts of myself. It was a deeply spiritual experience that is difficult to put into words. It did bring me to a place where I was almost one with the pain and did not perceive it as “bad.”
I do remember fully “coming back” into the room 2x when I got an actual break (a few minutes) from contractions. I am unsure if I would have had as deep of an experience if I had experienced a normal contraction pattern. I may have gotten too distracted by my surroundings and the people around me. In some ways I am grateful that I was able to maintain my otherworldly mindset. I believe I had the journey I was meant to.
I don’t remember much. However, I did have the sense that things were not progressing as fast as those around me had anticipated. Eventually there was a discussion about if I would consent to having my waters broken. I delayed for a bit, but eventually consented. However, it was difficult to switch positions due to the fact that my contractions were fairly continuous. I sometimes felt like I had only seconds between contractions which wasn’t enough time to understand where I was going and get there. Before I could get into the position to have my waters actively released they broke spontaneously.
I was pleased with this, however my water was slightly meconium stained. My midwife assured me that this wasn’t necessarily terrible, but it did mean I was no longer a candidate for intermittent monitoring. The continuous monitor made moving away from the hospital bed, into the shower etc. much more difficult to do. I didn't really leave the vicinity of the bed after this point but I did continue to utilize position changes within the realm of the bed. I also began to feel an urge to push. I had decided prior to labor that I did not want constant cervical checks, however I was willing to consent to a check prior to pushing. I had a check shortly after my water broke and was only at 8cm and was not given the go ahead to push. I remember just trying to “breath the baby down” in a way that wasn’t “pushing” but was also honoring my body’s intuitive desires. This period of time was more physically intense than the time prior to it. I went even deeper into myself and also utilized a good bit of nitrous oxide. It was just a bit too convenient since both it and I were pretty much attached to the bed.
According to my doulas notes I reported an even stronger desire to push around 9:15pm and consented to another cervical check. This time I was 10 cm dilated and given the go ahead to officially begin pushing.
My Pushing Experience
There is a lot of discussion about how to push in the pelvic health space. I think part of that is there are a lot of public misconceptions about the role of the pelvic floor and what the pushing phase should look like. Some women have the idea that their pelvic floor pushes the baby out. This is untrue. Your uterus pushes the baby out, your pelvic floor needs to be able to lengthen to get out of the way. I think in order to counter the misconception some imply that the labor and delivery process should require little physical effort.
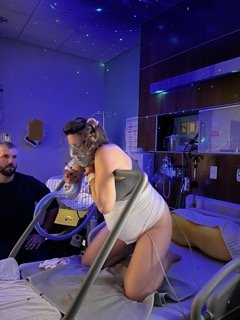
Pushing with my friend Nitrous Oxide.
Also, my doula did a great job setting the ambiance in the hospital.
Prior to entering the pelvic health space my only exposure to labor and delivery was what I saw on TV. This is often betrayed as an act of lying on your back, screaming or what is deemed “purple pushing”. Entering labor I was well aware of the downsides of pushing in this manor including increased tearing, increased risk of stalling etc.
I fully pictured myself pushing out of bed, squatting or on hands and knees. I hoped that because I had done some predatory work my pushing phase would be on the short side. My reality ended up being a bit different.
I pushed for three hours. I started the pushing process very aligned with how I envisioned it. Although I was in bed I was able to stay off my back and mostly push with an open glottis.
The situation was somewhat complicated by the presence of the meconium in my waters. Protocol dictated that the NICU team would be present at the time of delivery secondary to the potential need for respiratory support. They were called in at one point when I was pushing and quickly became impatient. I did not mind their presence. However, when the one NICU nurse tried to coach me to purple push because she perceived my pushing pattern to be “chaotic" I apparently told her to “get out”.
I don’t remember that per se. However, I do remember that at the time I felt that I was communicating with my baby who was scared to enter the world. In my altered mental state soothing her fears felt much more important than organizing my pushing pattern. I also believe that part of the reason my pushing looked odd was because my contractions continued to be weird and variable.
Eventually the dialogue with my baby ended and I could sense that she was ready to come. However, my open glottis pushing simply did not seem to be resulting in much progress. I don’t remember being particularly concerned. However I could sense that those around me were becoming anxious that I would become too tired to continue. There was also some intermittent concern over the baby's heart rate.
I knew that I did not want things to end with an emergency c-section.
The Delivery
I am unsure if I asked my midwife for some coaching or if I simply consented to her suggestions. Either way, my midwife suggested that I begin to push with a closed glottis. She assured me that she didn’t want me to “purple push” but rather just generate a tad bit downward force. I agreed. This method was more effective in moving the baby down. I was continuing to change positions. Eventually she suggested that I lay on my back with my doula and husband helping to flex my hips so that my sacrum would be free to open. In this position I was eventually able to deliver Annika’s head.
Upon doing so it became evident that her shoulder was stuck in my pelvis. I was instructed to stop pushing and a whole team of people were suddenly at my bedside. I knew that shoulder dystocias had the potential for bad outcomes. I sensed that the best thing I could do is stay calm, trust those around me and allow them to lead me through this time.
Annika was delivered after several manual maneuvers performed by my midwife and team. The total time from head to body was two minutes.
Up to this point my “birth intentions” were pretty well honored.
This is the point where those intentions kinda went to shit.
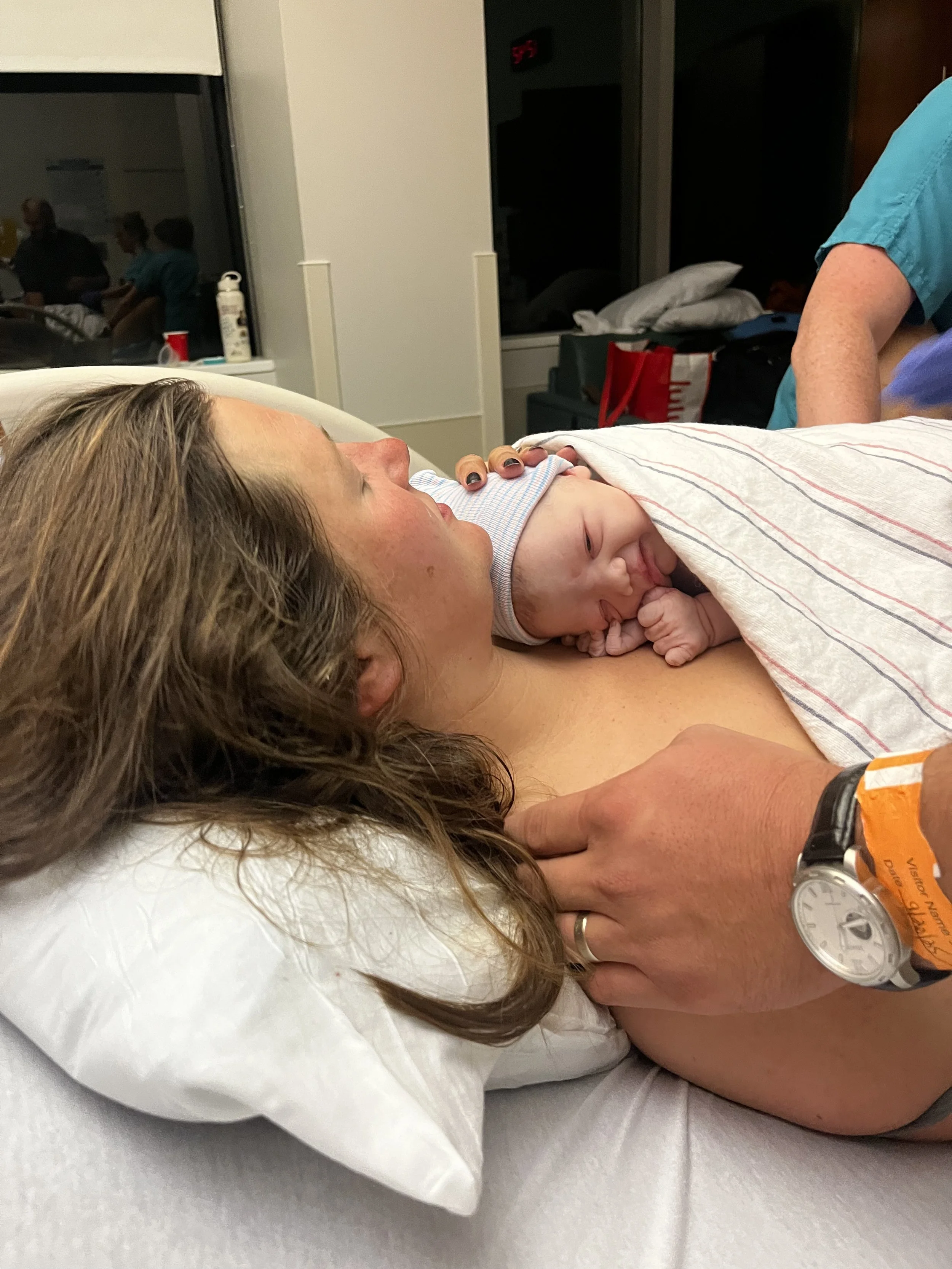
She was placed on my chest for a short moment before her cord was cut at one minute and she was taken to the side to be fully evaluated. The team did a great job of evaluating her in the room and bringing her back to me. According to the pictures provided by my doula, she was back on my chest within 10 minutes. For most of those 10 minutes I was busy delivering the placenta and making medical decisions for myself. However, it still felt like a really long time and certainly was not the golden hour that I hoped for.
Annika and I after she was evaluated by the NICU team.
I did opt to receive Pitocin post delivery. Due to the shoulder dystocia and the tearing that I had sustained I felt that the benefits outweighed the potential side effects.
Reflection on Labor and Delivery
I have had 6 months to reflect on this experience.
I know many people have traumatic birth experiences in which they felt their autonomy was completely taken from them.
I never felt that way. Did things go exactly as I hoped? No. However all of the medical intervention that I received felt appropriate and I never felt forced into anything.
I sometimes wonder if I prepared “well enough”. This has possibly been the hardest thing for me to sort out. Working in the pelvic health space there are a lot of professionals that proclaim to have programs that helped them achieve very short labors or pushing times. It is often insinuated that if you don’t have this experience the problem is preparation.
I believe that preparation is valuable. I believe exercise and movement can be helpful in positioning the baby and potentially leading to shorter labor times. I spent a fair amount of time and intention in this area. It was not, and still is not, my highest expertise. However, I did feel I had a good grasp on the concepts and had helped many clients prepare for labor with good results. Be that as it may, there were days I skipped my hip routine because the day got away from me. Frankly I felt so terrible in the first half of my pregnancy that I was a bit overwhelmed with all of the “catching up” I had to do in the second half to prepare for a baby in general. So I was not “perfect” in the birth prep area. Because of that, I do sometimes wonder if my outcome would have been “better” if I had done “better.”
I have to be okay not knowing. I also believe that there are some things that you simply can not control. Annika’s head was well above average in size at birth and has continued to measure above the 90th percentile through her pediatrician appointments. There was nothing I could do to have changed this. Maybe heeded my mother in laws warnings? She certainly didn’t get that big head from me!
I have also wondered if things would have been any different had I chosen a home birth. Would I have moved better? Maybe the shoulder wouldn’t have gotten stuck? Or maybe it would have and the outcome would have been worse. I don’t know. What I do know is when I was laying there with her head delivered and her shoulder stuck, I was grateful I had a whole NICU team at my bedside.
In a way there was something healing about receiving this medical intervention. I lost a lot (almost all) faith in the western medical system during my autoimmune journey. (link) There was something restorative for me about feeling safe in a hospital setting, having my intentions well honored, and only receiving care I truly needed.
The morning following delivery.
I believe that if I end up doing it again I would likely select the same team. I probably would prefer to deliver unmedicated again. I have considered if I would prefer an epidural. The biggest downside to being able to achieve such an otherworldly mindset was that I was pretty “out of it” immediately after delivery. I do wish I had clearer memories of the first time I saw her. In some ways I feel I was not all the way present. However, as I said earlier I do feel like I had the experience I was meant to.
In some cases you are encouraged to have a c-section in subsequent pregnancies following a shoulder dystocia. I am allowing myself not to think about this unless I truly need to.
My Postpartum Pelvic Symptoms
Despite my diligence with perineal massage I suffered a grade 3 perineal tear. For those of you unfamiliar with the grading of perineal tears… It means that I had tearing from the bottom of my vaginal opening all the way to my rectum. Truly fun times. Fortunately, most of my tearing was superficial involving my skin and some muscle sheaths but very little actual muscle.
September 22nd
The day we came home from the hospital.
Once again, as a pelvic PT, I was slightly disappointed not to have “been better” in this area. However, as someone who has been on the “tight side” from a pelvic floor perspective for at least as long as I have known I had a pelvic floor, I was pleased that the tearing didn’t extend far into the muscle. I felt that this in itself represented an improvement and was likely partially improved by the perineal massage. I also have the awareness that in the case of a shoulder dystocia things could have turned out much worse.
In addition to the tearing, I also had a good bit of pelvic organ prolapse immediately postpartum.
I had a history of cystocele (bladder prolapse) prior to becoming pregnant. I had no symptoms immediately prior to pregnancy, but did have some throughout pregnancy which I attributed both to hormonal changes and my inability to do the hypopressive maneuver during this time. These symptoms worsened following delivery.
I began self evaluating in standing with a mirror about 2 weeks postpartum. My bladder was more visible to me than it had ever been prior. Additionally, I also had a good bit of descent of my posterior wall/rectum. Although I had no history of rectocele I was not surprised to find that I had one following labor due to the extensive pushing and the tear being present. If I were to have rated my prolapse postpartum I would have said I had a grade 3 cystocele and grade 3 rectocele.
My subjective symptoms included post void dribble, which I was familiar with and had dealt with prior. Additionally I had significant pelvic heaviness. Although this is a common prolapse symptom I had never really experienced this prior.
My Postpartum Healing Mindset
My midwives elected to have the OB on call perform my stitching. I, unfortunately, was lucid for that part. I remember them explaining a bit about the tear to me. I remember reflecting that I was not worried about it. Explaining that I was a pelvic PT and had seen clients recover from worse. I had a deep belief that healing was possible and I was well resourced to help myself or seek outside guidance if needed.
My Postpartum Recovery
Stay tuned, I will be publishing my originally intended blog about my postpartum recovery soon.
Subscribe to my newsletter to be sure you don’t miss it!